Summary
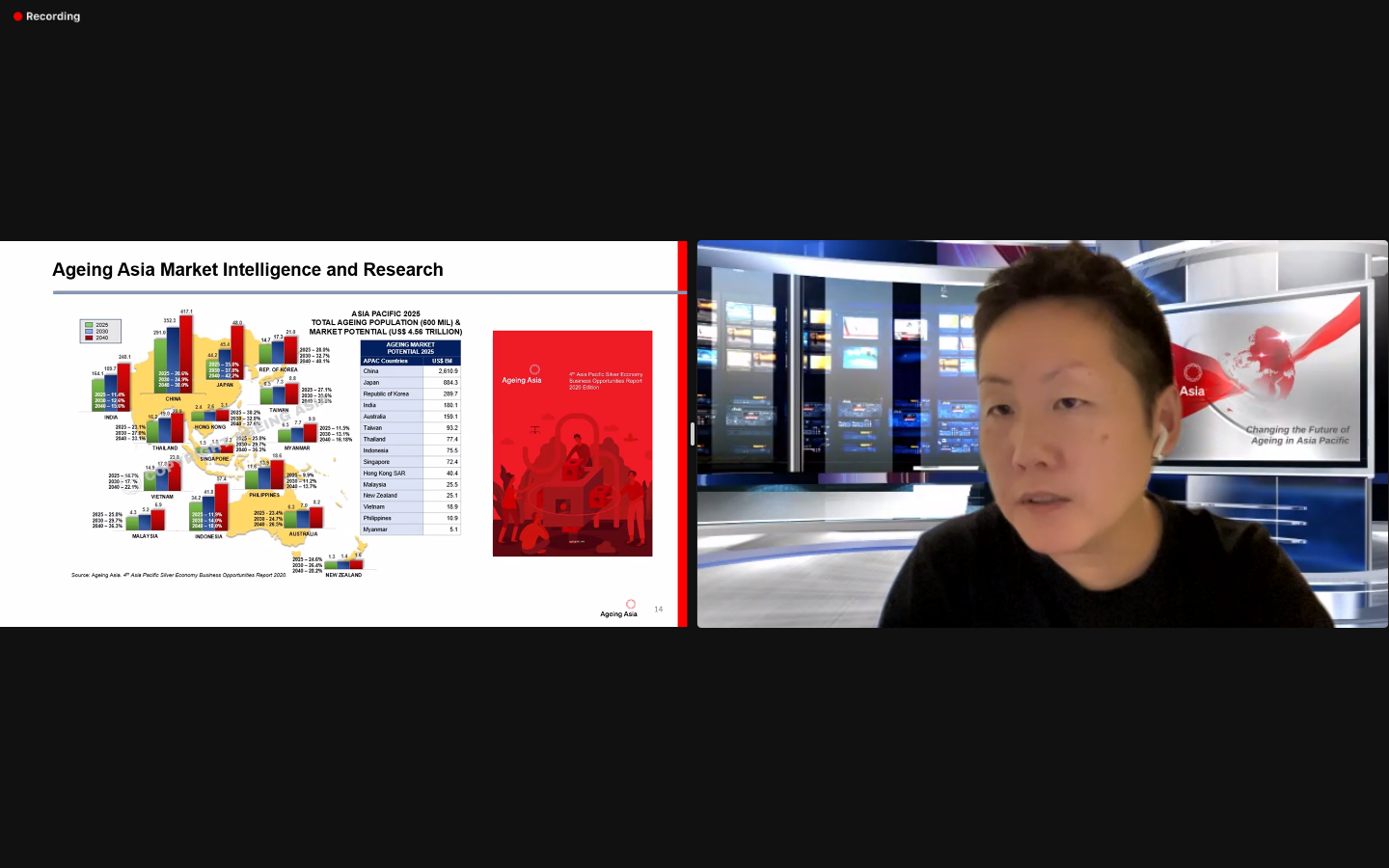
- Malaysia will transform from an ageing society to an aged society within the next few decades, with an estimated 17% of the population aged 65 and above by 2050.
- Ageing populations have significant economic and health impacts, including the increased incidence of infectious and chronic diseases, due to weakened immune systems and frailty.
- There is a critical need to ensure populations are healthy throughout the life-course through preventive measures, including life-course immunisation, so everyone can lead a productive and fulfilling life as they grow older.
- To discuss how public and private sector can continue to collaborate to promote the health of older adults through life-course immunisation, a roundtable was held with leading experts from various sectors, including policy makers, academics, clinicians, healthcare providers and healthy ageing advocates.
- Participants discussed the barriers faced to protect vulnerable populations, which include low vaccine confidence, perceived risk of side effects from vaccines, generic public health campaigns, lack of a champion to drive the needed changes, logistical and supply chain issues and a greater focus on treatment rather than prevention during consultations.
- Participants also discussed the critical need to raise awareness on the benefits of life-course immunisation, leverage existing initiatives and policies to incorporate life-course immunisation, increase touchpoints for vaccination to pharmacists and train healthcare professionals as advocates.
- This requires both a top-down approach, including the prioritisation of life-course immunisation at the national agenda on healthy ageing, as well as a bottom-up approach, including strengthened community-based efforts and private-public partnerships to support health and well-being of older adults.
Introduction
Globally, countries are experiencing a shifting demographic towards an ageing population and the challenges and opportunities that come with it. Older adults, referred to in this report as people aged 65 and above, comprise the world’s fastest growing age group due to increased life expectancy and declining fertility rates. In 2018, older adults outnumbered children under the age of five for the first time and by 2050, they will outnumber adolescents and youths aged 15 to 25.[i]
In Malaysia, the percentage of individuals aged 65 and above will increase from approximately 7% in 2022, to 17% in 2050, transforming the demographic status from an ageing to aged society.[ii] Consequently, the old-age support ratio, which refers to the number of people who are economically active to the number of older adults, will decrease from 8.4 in 2022 to 3.5 in 2050.
In addition, while individuals are living longer, they may not be living healthier. Even though life expectancy in Malaysia was 76 years in 2020[iii], on average individuals only spend 65.7 years of their lives in a healthy status.[iv] This means that individuals lose more than a decade of their lives if there are no healthy living interventions. Moreover, there will be a greater demand in healthcare and eldercare services to treat chronic and infectious diseases, as the likelihood of developing serious complications and even death increases as individuals age due to frailty and weakened immune systems. For example, influenza disproportionately impacts older adults globally, as older adults aged 65 and above account for up to 70% and 85% of influenza-related hospitalisations and mortality, respectively.[v] This means that there is an urgent need to keep populations healthy, to reduce the impact on a country’s healthcare resources and economic growth.
There is an opportunity for a coordinated response from policy makers, civil society, academic and the private sector to identify and advance innovative solutions to the healthcare systems, so that older adults can live fulfilling, healthy and productive lives at old age.
Recognising the challenges of this demographic shift globally, the United Nations has dedicated the years 2021–2030 as the Decade of Healthy Ageing,[vi] to improve the lives of older people, their families and communities. In Malaysia, the topic of healthy ageing has been articulated in various ministerial policy and development papers. In 2011, the National Policy for Older Persons was implemented by the Ministry of Women, Family and Community Development, which complemented efforts by the Ministry of Health’s National Health Policy for Older Persons in 2008.[vii] The policies aimed to empower individuals, families and communities to optimise their full potential and wellbeing in old age and encourage the participation in health promotion and disease prevention activities throughout the life-course, respectively.[viii]
“There is an outdated view that healthy ageing should only be considered post-retirement. It is however, a life-long journey that requires a shift in mindset in the community and at primary care level, to focus on strategic prevention of non-communicable diseases that can accelerate ageing.”
Prof. Dr Shahrul Bahyah binti Kamaruzzaman – Deputy Dean and Consultant Geriatrician, University of Malaya & President, Malaysian Healthy Ageing Society
To further future proof the healthcare system and address the challenges of an ageing population, the Malaysian government is proposing structural changes and a healthcare reform, including the shift from curative and treatment-focused care to creating a more proactive and preventive healthcare system.[ix] To achieve this vision, a paradigm shift in healthcare delivery is needed, including the utilisation of preventive measures, such as life-course immunisation, to address the needs of a growing ageing population and with it strengthen the resilience of the Malaysian healthcare system.
Leadings experts in the field of ageing and health, including policy makers, academics, clinicians, healthcare providers and healthy ageing advocates convened virtually on 12th July 2022 to align on progressive policy actions needed to prioritise life-course immunisation in healthy ageing discourse in Malaysia, specifically for influenza vaccines. This is the second in a series of roundtables organised across Southeast Asia – in Thailand, Malaysia and Vietnam – by Ageing Asia and supported by Sanofi.
The roundtable is timely, given recent reports of influenza outbreaks in Malaysia, due to the reopening of international borders and loosening of COVID-19-related restrictions, which increased social activities.[x] The roundtable was an opportunity for stakeholders to discuss ways to improve the access to and uptake of life-course immunisation in Malaysia to reduce the incidence and impact of such outbreaks from vaccine-preventable diseases.
In addition, this roundtable in Malaysia built on insights first discussed in a report published by the EU-ASEAN Business Council, KPMG and Sanofi, ‘The Decade of Healthy Ageing in ASEAN: Role of Life-course Immunisation’ in 2021[xi], as well as a focused roundtable on ‘Influenza Vaccines for the Elderly: A Necessity or an Option?’ in March 2022. These initiatives focused on the urgency of implementing a life-course approach to immunisation and the actionable solutions that can be taken by governments, private sectors and communities.
All discussions have been summarised in this report, with no direct attribution to any participants. However, contributing participants and organisations have been credited to these highlights.
We thank all roundtable participants for their valuable contributions.
The benefits of life-course immunisation for healthy ageing
Life-course immunisation is a strategy to keep populations healthy and further strengthen the resilience of healthcare systems. It is the uptake of vaccination at all stages of life, from childhood to old age, and an approach to vaccination that responds to an individual’s lifestyle and specific vulnerabilities to infectious diseases. Immunisation is one of the most effective public health interventions that prevents up to five million deaths annually and can be utilised to ensure healthy ageing.[xii] It protects against vaccine-preventable diseases and its associated complications, as well as worser complications from infection in vulnerable populations, including older adults with chronic diseases.
For example, vaccine-preventable lower-respiratory infections, such as influenza and pneumococcal pneumonia, disproportionately affect older adults and were the third leading cause of death among those aged 70 and above in 2019.[xiii] Take influenza as an example, old age is a risk factor for poorer outcomes from infections due to weakened immune system and declining health – there is a 10% risk of developing complications, including hospitalisation, intensive care unit admissions or death, in individuals aged 25 to 60 but 28% risk in older adults.[xiv] People are six times more likely to have acute myocardial infarction within a week following influenza infection, especially among older adults.[xv]
The COVID-19 pandemic also revealed the increased risk of adverse outcomes among older adults, with 24.8% of mortality cases attributed to individuals aged 65 and above.[xvi] In addition, there were a four-times increased risk of receiving invasive mechanical ventilation and two-times increased risk of mortality in individuals who are infected with both influenza and COVID-19.[xvii]
Therefore, vaccination especially for the elderly are important to safeguard their health both during and outside of a pandemic. The uptake of vaccinations can reduce the cost of medical treatments for vaccine-preventable diseases and its associated complications. Moreover, healthcare systems can redirect resources to areas of prioritisation, such as tackling non-communicable diseases.
Life-course immunisation landscape for older adults in Malaysia
Malaysia does not have a population-wide adult immunisation programme, as the National Immunisation Programme currently focuses on childhood vaccination. The Ministry of Health in Malaysia has a list of recommendations for adult immunisation, including for high-risk groups, such as older adults and those with chronic conditions.[xviii] For example, annual vaccination against influenza is recommended for all individuals aged 6 months and above throughout the year. The third edition of the guidelines from the Malaysian Society of Infectious Diseases and Chemotherapy further recommends annual influenza vaccinations for older adults in nursing homes and hospital wards.[xix] While these recommendations exist, they are not widely conveyed or implemented, as they are not mandatory nor provided for free or subsidised.
On the supply and provision of vaccines, amidst the COVID-19 pandemic, every household was eligible for tax exemption up to RM1,000 for vaccination, including for influenza, pneumococcal, tetanus and the COVID-19 vaccines.[xx] Beyond this, there is currently no national budget allocated to provide older adults with free vaccinations, therefore, these costs are entirely borne out-of-pocket or dependent on the private sector, including employee health benefits and private health insurance. At present, influenza vaccination is provided mainly by medical practitioners in the private sector, which can be inaccessible to many individuals.[xxi] Only 10% of adult vaccinations are administered in the public sector if individuals have other chronic conditions that increase the risk of infections[xxii] and Malaysia has one of the lowest vaccination rates in the Southeast Asian region.[xxiii]
Despite the apparent benefits of vaccination, the uptake beyond childhood vaccination is low in Malaysia. For example, the estimated coverage of influenza vaccination among adults is 3%.[xxiv] This is still far below the coverage rate in other ASEAN Member States and the target set out by the World Health Organization at 75% to prevent annual epidemics.[xxv] With an increasing proportion of ageing adults, there is an opportunity for government, private sector and communities to prioritise initiatives and policies to enable healthy ageing, including the integration of life-course immunisation in the healthy ageing agenda, to ensure that older adults can lead productive and fulfilling lives throughout all ages.
What are the barriers faced to protect vulnerable populations, including the elderly in Malaysia?
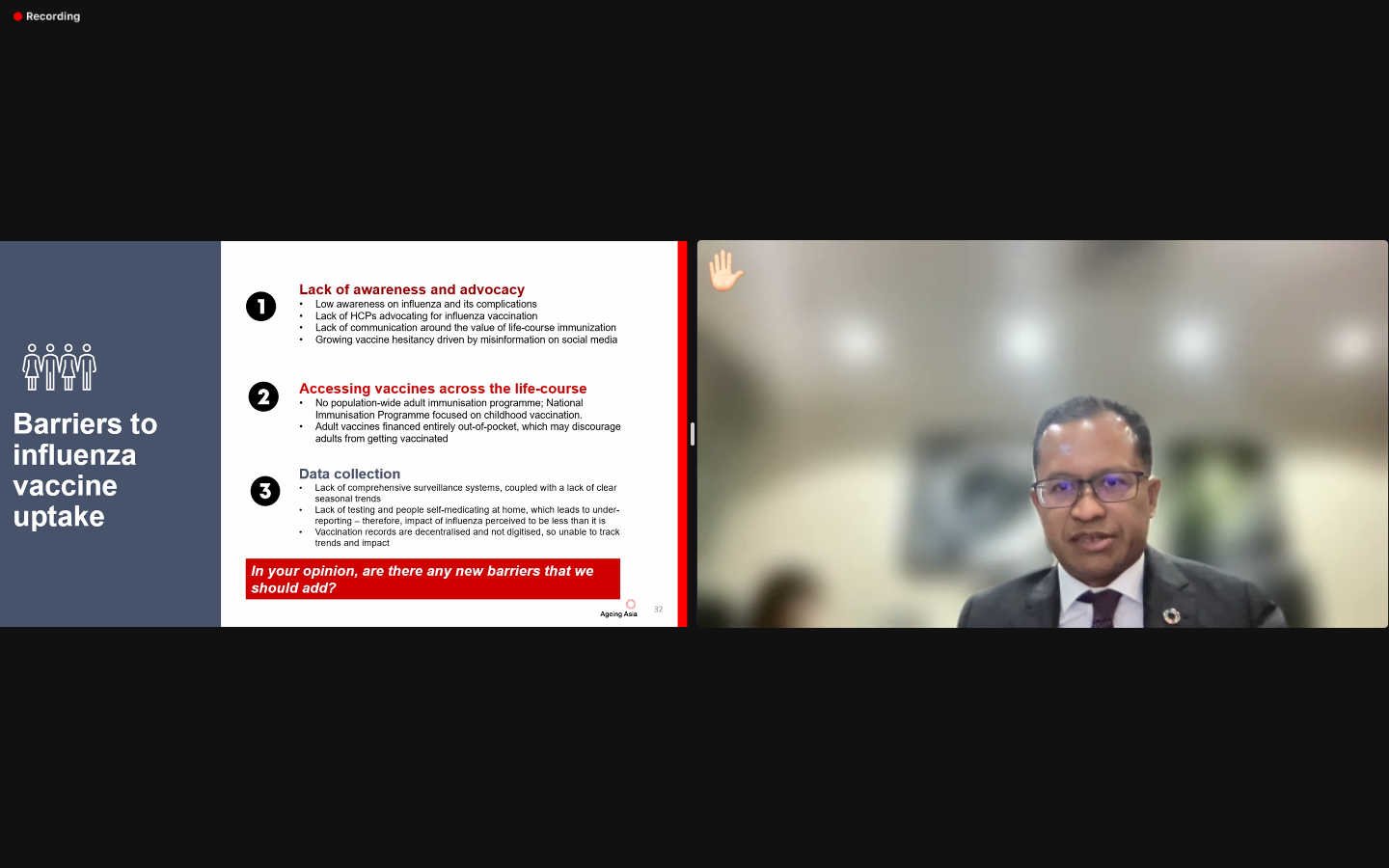
Awareness of the benefits of life-course immunisation
Low awareness among the general public
Older adults are wary of the side effects of vaccination, especially if two vaccines are taken within a close period or at the same time. This was evidenced during the COVID-19 pandemic, as each household were offered tax exemptions to also obtain free influenza vaccinations, but the uptake of influenza vaccines was low. Misinformation on the Internet further exacerbates low vaccine confidence and subsequently, discourage its uptake.
Anecdotes revealed that many older adults who were willing to take the influenza vaccine were mainly English-speaking individuals, which exemplified that awareness on the benefits of immunisation were effectively targeted to the English-speaking population but were not as effective in other populations, including those who speak Malay, Mandarin, Tamil and other languages and dialects.
In addition, influenza is commonly seen as no different from the common cold and not perceived as a serious threat. Consequently, older adults do not perceive influenza vaccination to be an important aspect to promote good health and well-being.
Accessibility of vaccines
Supply chain and logistic challenges
Even though primary care clinics have the capability of providing vaccination to older adults, logistical issues exist, including the lack of supply of vaccines or lack of regional cooperation and integration between the private and public sector to utilise available capacity. The cold-chain management and storage capabilities for vaccines could be strengthened, so vaccines are stored appropriately, from manufacture and transportation to storage stages, and to avoid wastage.
Insufficient access points in community settings
At present, community pharmacists are unable to administer vaccines. Even though pharmacists can raise awareness on the benefits of life-course immunisation, they would need to refer individuals who are interested to visit their local general practitioners or public hospitals to access the vaccines, increasing multiple touchpoints for individuals, which may discourage the uptake of vaccination.
Advocacy and action to promote the uptake of vaccination
Absence of coordination and integration within communities
Unlike countries such as Singapore, where there exist regional health clusters that are dedicated to specific populations based on their geography, populations in Malaysia access any clinics based on convenience and preference. Therefore, there is a lack of integration and partnership with local communities and organisations to provide programmes and services to ensure older adults can age healthily and more importantly, to communicate and advocate for the benefits of life-course immunisation at the local level.
Lack of advocacy from healthcare professionals
Healthcare professionals are primary and trusted sources of information for many. However, on-ground sentiments show that many healthcare professionals do not actively advocate for immunisation, especially at the primary care level. This is due to insufficient time to discuss the importance of preventive measures, including immunisation, with the patients. Rather, consultations were focused on treatments and existing diseases.
Lack of policy action on adult immunisation programmes
While the impact of vaccine-preventable diseases on older adults is clear, Malaysia has yet to recognise the importance of life-course immunisation within healthy ageing – the country does not yet have a National Immunisation Programme beyond paediatric immunisation. Malaysia has one of the most extensive paediatric immunisation programmes – the programme is based on the World Health Organization (WHO) Expanded Programme on Immunization (EPI). The EPI recommends that all countries immunise against 6 childhood diseases; however, Malaysia has expanded its NIP to 12 major childhood diseases.[xxvi] The Malaysian government’s investment into and recognition of the importance of paediatric immunisation has resulted in high vaccine coverage rates of around 95%[xxvii] – a recognition that could well reap the same high uptake rates, if implemented across life-course immunisation as well. However, due to a stronger focus on tackling the rising prevalence of non-communicable diseases in Malaysia, there could be a potential lack of funding and resource allocation towards a population-wide life-course immunisation programme.
What can be done to better protect vulnerable populations, especially the elderly in Malaysia?
To further complement existing efforts by the government in promoting healthy ageing and future proofing the healthcare system through a stronger emphasis on preventive care, the recognition of life-course immunisation as an important pillar of healthy ageing, as well as cross-sectoral collaboration is urgently needed in three categories:
- Raise awareness on the benefits of life-course immunisation – Awareness
- Ensure adequate and efficient access to life-course immunisation – Access
- Advocate for the uptake of life-course immunisation – Action
This requires both a top-down approach, including the prioritisation of life-course immunisation at the national agenda on healthy ageing, as well as a bottom-up approach, including strengthened community-based efforts and private-public partnerships to support health and well-being of older adults.
Raise awareness on the benefits of life-course immunisation
Recognition of life-course immunisation as a critical pillar within healthy ageing discourse and policies from the government
The Malaysian government has included healthy ageing as a public health strategy in the upcoming proposed structural reforms of the healthcare system to ensure that the discourse is prioritised at the national level. This is a significant step in recognising the challenges of an ageing population, and this strategy could be further leveraged by incorporating life-course immunisation as a core healthy ageing pillar to safeguard population health. Examples of initiatives include commissioning return-on-investment or health economic studies in Malaysia to determine the cost-benefit analysis of life-course immunisation for older adults, so policymakers have concrete evidence-based recommendations to support policy actions, as well as open public-private partnerships to build vaccine confidence and raise awareness on the benefits of life-course immunisation.
There is an opportunity to take learnings on the development, implementation and monitoring of the Expanded Programme on Immunisation for children. A major factor that contributed to the successful coverage rate of vaccination and reduction in mortality rates in children is due to sustained advocacy recognition of the importance of childhood immunisation from the Malaysian government, as well as open multistakeholder partnerships, such as initiatives with religious bodies to tackle vaccine hesitancy. Similar proactive and initiative-driven advocacy can be applied to a programme that targets individuals throughout the life-course, which starts with the recognition of the benefits of life-course immunisation.
Recognition of the benefits of life-course immunisation within population health
Due to the low vaccine confidence, a concerted effort to communicate the health and economic benefits of life-course immunisation for individuals, families and communities is needed, especially on impact of infectious diseases and misconceptions about vaccinations. For example, a mindset shift about life-course immunisation, not as a cost but an investment in the long-term promotion of health and well-being, is needed and could be incorporated into early years school education.
These communication efforts should be targeted and consider the different languages and dialects of populations and utilise the most effective channels, such as social media platforms, to reach them.
Ensure adequate and efficient access to life-course immunisation
Financing life-course immunisation programmes
Ensuring adequate national budgets are allocated to life-course immunisation could be strengthened through leveraging existing national policies on healthy ageing and incorporating a stronger emphasis on life-course immunisation. A creative and flexible approach to financing immunisation programmes could be explored through co-payments and pooled funding from the private sector.
Leveraging and strengthening existing technology
The MySejahtera application, which was developed by the government to monitor outbreaks and uptake of vaccines during the COVID-19 pandemic, is currently expanding its functionality to include a non-communicable disease risk test and integrate the National Immunisation Program. The application could be further leveraged to include the recommended adult immunisation, so older adults can easily access their medical history and be reminded to obtain vaccinations. In addition, the application can provide a source of data to track and monitor the uptake of vaccines, beyond the COVID-19 vaccine, to better inform long-term vaccine procurement, which ensures adequate supply to meet population demand.
Addition of access points for individuals through pharmacies
The inclusion of pharmacists as an additional touchpoint for vaccination increases convenience and access for populations at the community level. Currently, while pharmacists can advocate for life-course immunisation, they are not permitted to administer the vaccine. As such, there is no continuity of care and their referral to a primary care physician further discourages and inconveniences older adults from accessing these vaccinations. Therefore, legislative changes to ensure pharmacists could administer vaccinations, as well as their training, are needed to tackle this bottleneck.
Advocate for the uptake of life-course immunisation
Leverage healthcare professionals as advocates
The Immunise4Life initiative was launched in 2013 by the Ministry of Health, the Malaysian Paediatric Association and the Malaysian Society of Infectious Diseases and Chemotherapy to combat vaccine hesitancy and drive greater awareness on vaccine-preventable diseases and the benefits of life-course vaccination. There are currently toolkits to equip healthcare professionals to discuss immunisation for at-risk populations, including pregnant individuals and those who are travelling overseas. There is an opportunity to expand this initiative and create a toolkit tailored for older adults, so healthcare professionals understand the specific concerns of this population and benefits of life-course immunisation for healthy ageing. To complement such initiatives, training courses could be designed for healthcare professionals to equip them as advocates for life-course immunisation.
Multi-stakeholder collaboration to champion and sustain life-course immunisation
Finally, participants discussed the necessity of having a central body or association that continuously champion the cause of life-course immunisation and bring together various stakeholders to devise a concerted, multi-stakeholder effort.
Conclusion
Healthy ageing is beyond a health issue and cross-sectoral collaboration is critical between areas of social development, economy and health to develop a holistic and comprehensive national policy that “ensures healthy lives and promotes well-being for all at all ages” (Sustainable Development Goal 3) and that the visions of the Decade of Healthy Ageing are met. Life-course immunisation, part of the Immunization Agenda 2030, is an important pillar to reach these goals, as it safeguards against vaccine-preventable diseases and complications from infections in older adults, as well as reduces complications due to chronic diseases. To further complement existing efforts by the government, continued and strengthened provision of adult vaccinations by the private sector, as well as community-level engagement is needed to champion and advocate for life-course immunisation for healthy ageing.
“While initial investments into expanding the National Immunisation Program for adults may be high, the returns will be significant in terms of population health, savings for the healthcare system and economic productivity.” Dr Khor Swee Kheng – Chief Executive Officer, Angsana Health
(English report) Healthy Ageing and Life-Course Immunisation Policy Dialogue Series – Thailand
| Attendees (in alphabetical order) |
| · Dr Chong Su-Lin – Chief Executive Officer, IMU Healthcare
· Mr Chris Hardesty – Moderator · Dr Feisul Mustapha – Deputy Director for Non-Communicable Diseases, Ministry of Health · Mr Jack Shen Lim – Business Development and IT Director, Tigas Alliance · Ms Janice Chia – Ageing Asia · Dr Kejal Hasmuk – Geriatrician, University of Malaya · Dr Khor Swee Kheng – Chief Executive Officer, Angsana Health · Dr Kong Why Hong – Founder, AIM Healthcare Acupuncture TCM Centre & iElder Asia · Ms Lovy Beh – Senior Vice President, BP Healthcare Group · Dr Molly Cheah Bee Li – President, Gerontological Association of Malaysia · Dr Safurah binti Haji Jaafar – Associate Professor, Department of Community Medicine, International Medical University Malaysia · Prof. Dr Shahrul Bahyah binti Kamaruzzaman – Deputy Dean and Consultant Geriatrician. University of Malaya & President, Malaysian Healthy Ageing Society · Dr Tan Hui Ling – Managing Director, Bagan Specialist Centre · Prof. Dr Zamberi Sekawi – Malaysian Influenza Working Group · Mr Aidi-Affendi Kusim – Sanofi · Ms Ada Wong – Sanofi · Ms Doreen Tan – Sanofi · Ms Elaine Yeap – Sanofi · Mr Sri Murali Sivadason – Sanofi |
References
[i] United Nations Department of Economic and Social Affairs. 2019. World Population Prospects 2019: Highlights. [Online]. Available from: https://population.un.org/wpp/Publications/Files/WPP2019_Highlights.pdf. [Accessed July 2022].
[ii] United Nations, Department of Economic and Social Affairs, Population Division. (2019). Probabilistic Population Projections Rev. 1 based on the World Population Prospects 2019 Rev. 1. [Online]. Available from: http://population.un.org/wpp/
[iii] The World Bank. (2022). Life expectancy at birth, total (years) – Malaysia. [Online]. Available from: https://data.worldbank.org/indicator/SP.DYN.LE00.IN?locations=MY [Accessed June 2022].
[iv] World Health Organization. (2020). Healthy life expectancy (HALE): Data by country. [Online]. Available from: https://apps.who.int/gho/data/node.gisah.HALE?lang=en [Accessed July 2022].
[v] Centers for Disease Control and Prevention (CDC). (2022). Flu & people 65 years and older. [Online]. Available from: https://www.cdc.gov/flu/highrisk/65over.htm [Accessed July 2022].
[vi] World Health Organisation. (2020). UN Decade of Healthy Ageing: 2021-2030. [Online]. Available from: https://www.who.int/initiatives/decade-of-healthy-ageing [Accessed June 2022].
[vii] Radhi NAM & Arumugam T. (2019). Are we ready for an ageing Malaysia? New Straits Times. [Online]. Available from: https://www.nst.com.my/news/exclusive/2019/12/548012/are-we-ready-ageing-malaysia [Accessed July 2022].
[viii] Sulaiman WAW. (2019). Policies on the health of older adults in Malaysia. Regional workshop on integrating policy and research on ageing in ASEAN. [Online]. Available from: https://www.duke-nus.edu.sg/docs/librariesprovider3/education-docs/1)-policies-on-the-health-of-older-adults-(malaysia)-by-dr-wan-aliaa-wan-sulaiman.pdf?sfvrsn=a681a329_4 [Accessed July 2022].
[ix] New Straits Times. (2022). Khairy: White Paper to put Malaysian health system on sustainable footing. [Online]. Available from: https://www.nst.com.my/news/nation/2022/06/804028/khairy-white-paper-put-malaysian-health-system-sustainable-footing [Accessed July 2022].
[x] Murugesan M. (2022). #HEALTH: Remain vigilant against influenza. New Straits Times. [Online]. Available from: https://www.nst.com.my/lifestyle/heal/2022/07/811452/health-remain-vigilant-against-influenza [Accessed July 2022].
[xi] EU-ABC, KPMG, Sanofi and WPPF. (2021). The Decade of Healthy Ageing in ASEAN: Role of Life-course Immunisation. [Online]. Available from: https://healthyageingasean.org. [Accessed June 2022].
[xii] World Health Organization. (2019). Immunization. [Online]. Available from: https://www.who.int/news-room/facts-in-pictures/detail/immunization [Accessed June 2022].
[xiii] Viz Hub. (2022). GBD Compare. [Online]. Available from: https://vizhub.healthdata.org/gbd-compare/ [Accessed June 2022].
[xiv] Pui LW, Hoe LS, Chun KP, et al. (2020). The effects of age on clinical characteristics, hospitalization and mortality of patients with influenza‐related illness at a tertiary care centre in Malaysia. Influenza and other respiratory viruses. 14(3): 286-293.
[xv] Kwong JC, Schwartz KL, Campitelli MA, et al. (2018). Acute myocardial infarction after laboratory-confirmed influenza infection. The New England Journal of Medicine. 378: 345-353.
[xvi] Ismail SNA, Zaki IAH, Noordin ZM, et al. (2022). Clinical characteristics and risk factors for mortality in patients with COVID-19: A retrospective nationwide study in Malaysia. Proceedings of Singapore Healthcare. 31: 1-8.
[xvii] Swets MC, Russel CD, Harrison EM, et al. (2022). SARS-CoV-2 co-infection with influenza viruses, respiratory syncytial virus, or adenoviruses. The Lancet Correspondence. 399 (10334): 1463-1464.
[xviii] Ministry of Health Malaysia. (2022). Immunization schedule for the elderly. [Online]. Available from: myhealth.gov.my/en/immunization-schedule-for-the-elderly/ [Accessed July 2022].
[xix] Malaysian Society of Infectious Diseases and Chemotherapy. (2020). Guidelines for adult immunization: 3rd edition. [Online]. Available from: https://adultimmunisation.msidc.my/read-book/ [Accessed July 2022].
[xx] CodeBlue. (2020). Families can get RM1,000 tax exemption for vaccines: Minister. [Online]. Available from: https://codeblue.galencentre.org/2020/12/17/families-can-get-rm1000-tax-exemption-for-vaccines-minister/ [Accessed July 2022].
[xxi] BERNAMA. (2022). Influenza set to make a comeback in Malaysia. The Malaysian Reserve. [Online]. Available from: https://themalaysianreserve.com/2022/04/25/influenza-set-to-make-a-comeback-in-malaysia/ [Accessed July 2022].
[xxii] EU-ABC, KPMG, Sanofi and WPPF. (2021). The Decade of Healthy Ageing in ASEAN: Role of Life-course Immunisation. [Online]. Available from: https://healthyageingasean.org [Accessed July 2022].
[xxiii] Kamaruzzaman SB, Pang Y-K, Sekawi Z, et al. (2021). Perspectives on influenza in older adults in Malaysia: Insights into action on vaccination for high-risk adults. Ipsos. [Online]. Available from: https://www.ipsos.com/sites/default/files/ct/publication/documents/2021-06/Final_Perspectives%20Paper%20of%20Flu.pdf [Accessed July 2022].
[xxiv] Kamaruzzaman SB, Pang Y-K, Sekawi Z, et al. (2021). Perspectives on influenza in older adults in Malaysia: Insights into action on vaccination for high-risk adults. Ipsos. [Online]. Available from: https://www.ipsos.com/sites/default/files/ct/publication/documents/2021-06/Final_Perspectives%20Paper%20of%20Flu.pdf [Accessed July 2022].
[xxv] World Health Organization. (2003). Fifty-sixth World Health Assembly: WHA56.19: Agenda item 14.14: Prevention and control of influenza pandemics and annual epidemics. [Online]. Available from: https://apps.who.int/iris/bitstream/handle/10665/78320/ea56r19.pdf [Accessed June 2022].
[xxvi] Wong PL, Wong PF, Abu Bakar S. (2020). Vaccine hesitancy and the resurgence of vaccine preventable diseases: the way forward for Malaysia, a Southeast Asian country. Human Vaccines & Immunotherapeutics. 16(7): 1511-1520.
[xxvii] Immunisation Programme in Malaysia. Presentation at Vaccinology 2017 – International Symposium for Asia Pacific Experts. Available at https://www.fondation-merieux.org/wp-content/uploads/2017/10/vaccinology-2017-faridah-kusnin.pdf