In just 25 years from now, there will be more people over the age of 65 years in Asia than the total combined population of North America and the Eurozone. Unlike its Western counterparts, Asia has had a long-standing tradition of filial duty to care for its elders.
However, due to mass migrations, lower fertility, increased female participation in the workforce, and globalization, these long-held values are gradually beginning to change. Senior Asians are now more open to the idea of moving to a retirement or senior group living community.
A 2016 survey conducted in Singapore by the Lien Foundation showed that 50% of the respondents were willing to live in assisted living facilities.
While senior group living communities, like assisted living communities (ALFs), will begin to play a more significant role in the elder facility landscape, it is more than likely they will start to see similar challenges faced by their western counterparts. The first challenge is the chronic shortage of professional caregivers. The US, for instance, must recruit over 1.2 million employees by 2025 to meet the demands of its steadily growing senior population.
The second challenge is that the senior care system today is not designed to help prevent the onset of health issues in seniors, it is designed to “detect and treat”. For senior group living communities, this reactive approach can prove to be expensive and ineffective, especially when it comes to retaining residents for longer and ensuring their continued wellbeing. Without radically restructuring the approach to delivering senior care, senior housing operators will find it challenging to meet continually increasing demands.
Using AI devices for digital monitoring can make care more ‘proactive’.
The development of innovative digital healthcare technologies, such as Artificial Intelligence (AI), wearable health trackers and robotics, have begun showing reliable results and are making the case for shifting the senior care paradigm to be more proactive by augmenting caregivers and providing passive, remote monitoring.
LifeWell Senior Living Inc is a senior housing operator with nine communities across South Central and the Eastern United States. The group is a recognized leader in using leading-edge innovation to improve care for their residents. A study was undertaken on 500 seniors in six LifeWell communities across two states over a 24-month period to show whether the use of an AI-powered solution like CarePredict could improve the quality of resident experience and provide better health outcomes to residents while improving staff productivity. Of the six communities, CarePredict was installed and used at three of the communities and compared to a control group of three similar communities with similar resident demographics and geography but that did not install CarePredict.
(a) Improving the quality of resident experience:
In senior care, the first signs of declining health appear as changes in daily activity and behavior patterns. The ability to identify these changes well in advance is unprecedented. CarePredict uses a smart wearable, Tempo™, to autonomously collect the activity, location, and contextual data that identify daily activities of seniors such as eating, sleeping, cooking, walking, bathing, activity levels, and bathroom visits. The system then uses artificial intelligence and machine learning to establish a personalized baseline and flags residents who are out of their baseline, allowing staff time to intervene before the condition escalates to an actual issue.
The study showed that communities without CarePredict had a 58% higher fall rate than the communities using CarePredict. (The average fall rate – falls per head count was 2.12, compared with 1.34.)
Given that falls result in over 800,000 hospitalizations and 27,000 deaths in seniors annually, identifying whether a senior is at risk for falls can significantly impact hospitalizations and the length of stay in senior living communities.
The study also showed that the communities with CarePredict had a 21.3% lower hospitalization rate (34.5% hospitalization rate as opposed to 55.8% rate in communities without CarePredict.)
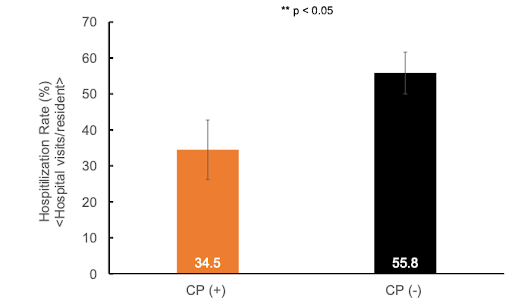
Fig 1
Reducing hospital admissions reduces resident turnover and increases the length of stay in the communities. CarePredict communities exhibited a 86-day increase in median Length of Stay (LOS), or a 67% increase compared to the control communities.
(b) Improved staff response time
The average time it takes the care staff to respond to residents’ requests for assistance is a good indication of the community’s ability to provide quality care and to understand whether the community has enough caregivers to assist residents. At the start of the study, the average time for staff to acknowledge a request from a resident was 610 seconds, and it was reduced to 360 seconds by the end of the two-year period. The time to reach the resident was reduced from 819 seconds to 600 seconds.
With state-of-the-art technology. CarePredict was used as a key differentiator in the marketing of their new senior housing communities and may have directly contributed to a more rapid occupancy ramp-up rate and final occupancy rates.
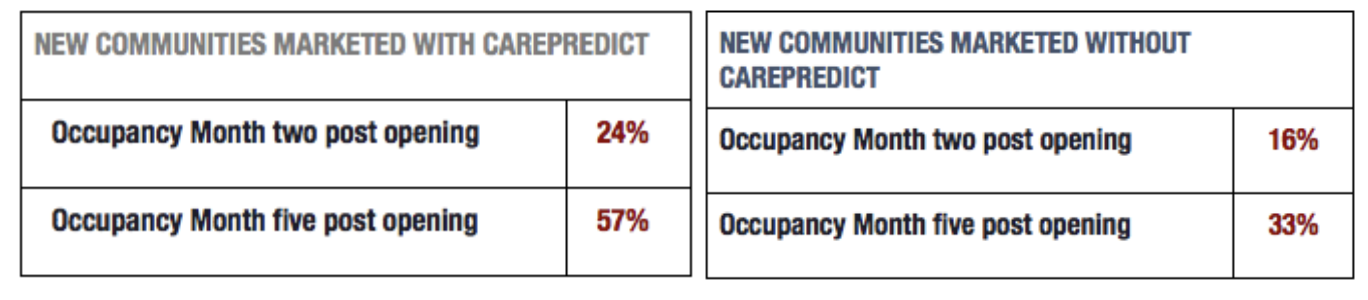
Fig 2
For the study, the average occupancy (%) for the six communities was computed by measuring the average community occupancy for the first five months post-opening. The average final occupancy rate for CarePredict communities was 90.3%, while the communities without CarePredict had 68.7%. CarePredict communities showed occupancy rates 7% higher than the national average for the US (83.6%.)
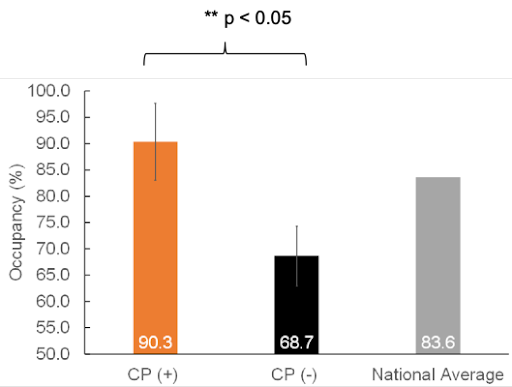
Fig 3
This commentary is by SATISH MOVVA, Founder & CEO, CarePredict Inc, a US Company
Satish has over 30 years of experience in health care technologies. He previously founded ContinuLink, an innovative Homecare and Hospice SaaS IT platform in the US. Prior to ContinuLink, Satish was the CIO of Sheridan Healthcare where he created the first mobile EMR device on a Palm Pilot in 1998 and the first SaaS EMR for Neonatal ICUs in 2000.
